Tackling Heart Health for Athletes
In 2023, college athletes Lebron James Jr. and Josh Davis suffered sudden cardiac arrest during team practices. According to the National Library of Medicine, sudden cardiac arrest is the leading cause of death for young athletes, and reports suggest that approximately 1 in 40,000 to 1 in 80,000 athletes die of sudden cardiac death each year.
Scott Shurmur, M.D., a cardiologist at the Texas Tech Physicians Center for Cardiovascular Health, shared his experience as a former collegiate athlete and expertise to address this growing health issue.

Scott Shurmur, M.D.
“It can be caused by a variety of things,” Shurmur said. “The most common cause is in a pathologic and abnormal thickening of heart muscle, called hypertrophic cardiomyopathy, found usually in one part of the heart, but not all of it. This can cause fatal rhythm problems that aren’t life-sustaining. Instead of beating regularly, normally efficiently, the heart just kind of wiggles and doesn’t supply enough blood to the body.”
Shurmur said that there are a number of leading conditions which cause cardiac failures. Hypertrophic cardiomyopathy is the most common, followed by an absent coronary artery and Brugada syndrome, a genetic condition that causes an irregular heartbeat.
Genetics and family history play a key role in cardiac issues in athletes, and they also can determine if athletes are able to play. “There is a very strong genetic component,” Shurmur said. “If there’s a family history of sudden death or survived arrests, then the workup starts, and the thickness of the heart muscle is a big key. Whether or not family members have died, how thick the heart muscle is a big key as well.”
Depending on the kind of athlete, the heart can experience two different physiologic adaptations. Shurmur mentioned that the heart gets bigger in an endurance athlete. For a resistance athlete, the heart gets thicker. This means that an endurance athlete at rest might have a lower resting heart rate because the heart accommodates extraneous physical activity.
Shurmur explained the difficulty for athletes to know if they are suffering from cardiac arrest in advance compared to non-athlete individuals. “There can be some shortness of breath, but in young, healthy people who are conditioned, usually there aren’t symptoms. The first symptoms are relatively catastrophic, and that’s one of the real difficulties.”
Shurmur acknowledged that certain supplements can be dangerous for the heart. He advised looking out for supplements like raw amino acids and creatine. He added that whey protein is a safe supplement for athletes to gain muscle mass.
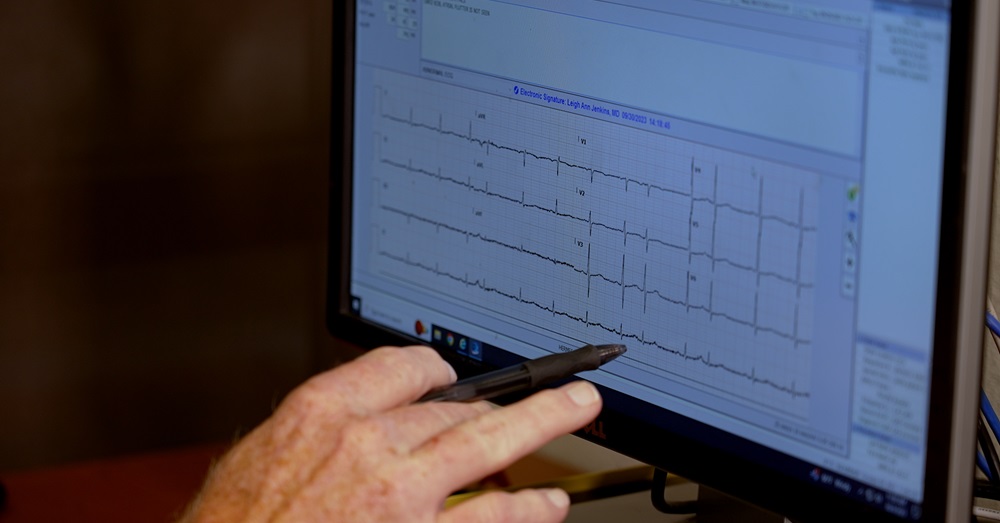
An EKG is a screening test that records the electrical signal from the heart
“Creatine, one has to be careful with, and the problem with any supplements is the FDA does not scrutinize them," Shurmur said. “Claims can be made about what’s in them, and other things can be in them. There can be things like anabolic steroids in them even though it appears nowhere on the label.”
Athletes should think more than short-term. Implementing something as simple as healthy hydration can save them now and long-term from heart issues.
“As you’re playing in your career, make sure you’re well hydrated,” Shurmur said. “Critical deficiencies in hydration can lead to passing out spells and loss of a couple specific minerals. Notably, magnesium and potassium can leave you at risk of a heart arrhythmia.”
An electrocardiogram (EKG) is a screening test that records the electrical signal from the heart to check different heart conditions. EKG screenings have gained a lot of push to be required for all competitive athletes at the high school level or higher. Shurmur clarified that an EKG isn’t necessary for every athlete but emphasized that every athlete needs a good history and exam with an experienced physician.
Related Stories
Labor of Love: More Women Turn to Nurse-Midwives for Healthcare
In hospitals, birth centers and private homes across the country, nurse-midwives are expanding women’s healthcare options.
Willed Body Memorial Service Honors Those Who Donated
The foundation of the TTUHSC Institute of Anatomical Sciences (IAS) was built on the university’s Willed Body Program. On Memorial Day each May, a service is conducted to pay respect to the Willed Body Program donors and their families.
Texas Tech University Health Sciences Center Garrison Institute on Aging Memory Clinic Recognized as an Age-Friendly Health System Participant
The Institute for Healthcare Improvement (IHI) has recognized the TTUHSC Garrison Institute on Aging Memory Clinic as an Age-Friendly Health System Participant.
Recent Stories
TTUHSC Experts Receive Junior Investigator Research Grants through Texas Alzheimer’s Research and Care Consortium
Texas Tech University Health Sciences Center (TTUHSC) researchers Aric Logsdon, Ph.D., and Jonathan Singer, Ph.D., received Junior Investigator Research Grants from the Texas Alzheimer’s Research and Care Consortium (TARCC).
CPRIT Awards TTUHSC Researcher $1.4 Million Cancer Grant in Efforts to Expand Rural Clinical Trials
The Cancer Prevention and Research Institute of Texas (CPRIT) awarded a $1.4 million grant to Erin Barr, M.D., a clinician of pediatric hematology/oncology and researcher in the School of Medicine at Texas TTUHSC. Barr’s research, “Enhancing access to pediatric oncology clinical trials in West Texas,” received funding under the Recruitment or Retention of Clinical Trialists Award.
Texas Tech University Health Sciences Center’s Klein Selected to Leadership Role by the Texas Pharmacy Association
The Texas Pharmacy Association announced (May 19) the appointment of Mary Klein, Pharm.D., as assistant vice president of Strategic Initiatives and Practice Innovation.
