Association of American Medical Colleges Releases Guide for Telehealth Competencies
TTUHSC’s Santos One of 16 National Experts to Draft Competency-Based Document
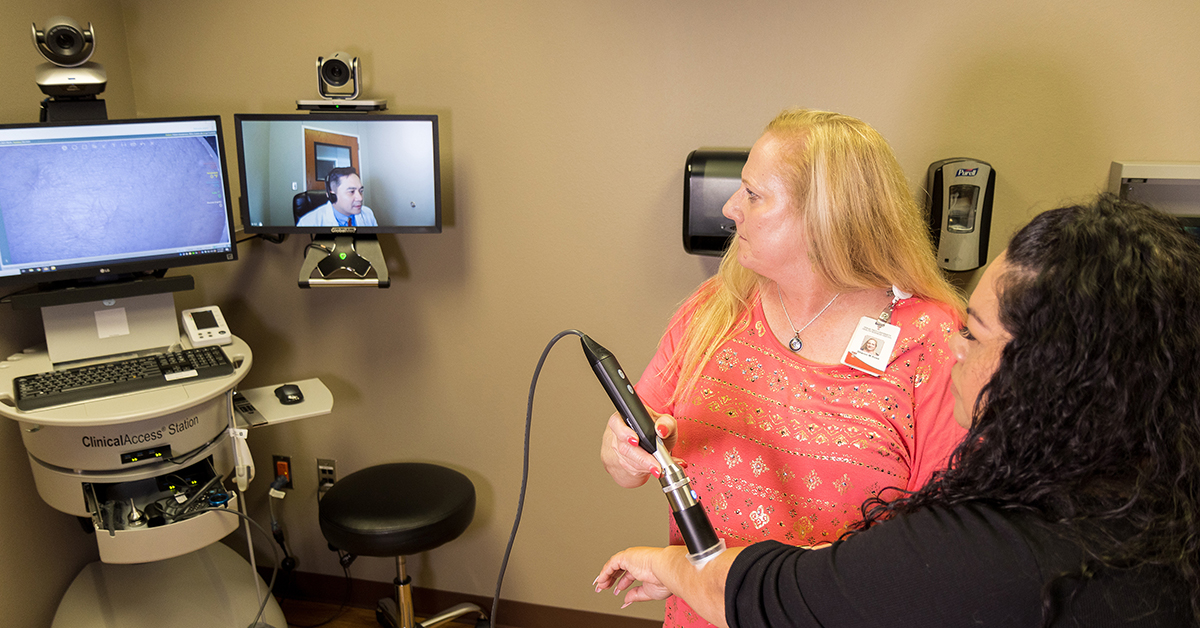
In the fall of 2019, Ariel Santos, M.D., MPH, joined 15 other telemedicine experts from across the United States as they convened in Washington, D.C. at the headquarters of the Association of American Medical Colleges (AAMC). Their goal was to develop a competency-based curriculum for telemedicine.
In March, approximately 18 months after the effort began, that goal was achieved when AAMC published, “Telehealth Competencies Across the Learning Continuum.” The guide, part of the AAMC series, New and Emerging Area in Medicine, is intended for people who develop curricula within the field of medicine and for those learning to practice or continuing their professional development.

Santos, an associate professor of surgery at the Texas Tech University Health Sciences Center (TTUHSC) School of Medicine and director of the university’s telehealth program, worked on the guide primarily as the principal investigator for the TexLa Telehealth Resource Center, a federally funded program that provides technical assistance and resources to new and existing telehealth programs in Texas and Louisiana.
Even before the pandemic, Santos said there was an uptick in telehealth activities because when appropriately used, telehealth, also known as virtual care, can potentially improve and maximize the delivery of health care. In addition to increasing access to health care, which it has done effectively during the pandemic, it can lead to improved patient outcomes, potentially decrease health care costs, lead to better overall patient experiences and increase physician satisfaction.
“With the increase in utilization of telemedicine, we need to make sure we have competency- and evidence-based education across the continuum of providers to ensure delivery of high quality virtual care,” Santos said. “It can standardize care, which can decrease liability and improve reimbursement as well improve the quality of care provided.”
Santos said competency-based education (CBE) or learning is a framework for teaching where students or learners advance from one learning level to higher based on their demonstration of knowledge and mastery of skills rather than time spent on a specific course. CBE is individualized, learner-centered and formative and emphasizes interprofessional communication, professionalism and system-based practice.
“CBE has improved health care since the focus is aligning the educational program with health system needs and priorities,” Santos explained. “We want to make sure our students are equipped with competencies — the knowledge, abilities and skills needed to function on a real life medical practice.”
Santos and his AAMC colleagues quickly identified several barriers to the large-scale adoption of telemedicine such as lack of resources, logistical costs, inadequate training, time and manpower shortages, poor reimbursement, regulatory restrictions and a lack of internet connectivity and broadband service. However, the unanticipated effects of the COVID-19 pandemic as it developed into a public health emergency benefitted and accelerated the adoption of telemedicine.

“Federal and state statutory changes, regulatory waivers and emergency orders have led to a significant scaling of telehealth services worldwide,” Santos added. “Also, telehealth became an essential tool to maintain access to health care because it helps reduce patient and provider exposure to the SARS-CoV-2 coronavirus, but primarily the lifting of regulatory restrictions is what has led to the increase use of telemedicine.”
Early on, many believed the use of telehealth would again subside as social distancing restrictions were eased. However, Santos said that is no longer the case because state and federal laws are currently being revised to encourage the wide adoption of telemedicine.
“The pandemic serendipitously helped telemedicine, but I think the adoption will continue considering our current lifestyle and demand for easy access,” Santos said. “With the improvement of technologies and wearables, there will be an increase in remote patient monitoring to address common illnesses as well as chronic conditions.”
Santos said that’s another reason why the new AAMC telehealth competencies guide is an essential tool. The competencies do not solely apply to medical students; they are just as relevant for trainees, practicing physicians and allied specialists as well.
“There is a need for competencies across the learning continuum,” Santos stressed. “This will help to develop a template of expectations and competencies needed to make sure we provide a standardized and high quality virtual care to our patients. I am hoping that we can adopt these competencies in our existing medical curricula, training and assessment. Hopefully, this will ensure that we will have competent, culturally sensitive and innovative physicians that will provide high quality virtual care to the society.”
Related Stories
38th Student Research Week Successful at Showcasing Secrets of Immune Defense
Student researchers at TTUHSC had the opportunity to showcase their presentation skills at the 38th Annual Student Research Week Feb. 25 – 27.
Celebrating Veterans: TTUHSC’s General Martin Clay’s Legacy of Service and Leadership
From his initial enlistment in the Army National Guard 36 years ago to his leadership in military and civilian health care management roles, Major General Martin Clay’s career has been shaped by adaptability, mission focus and service to others.
Texas Tech University Health Sciences Center School of Nursing Named Best Accelerated Bachelor of Science in Nursing Program in Texas
The TTUHSC School of Nursing Accelerated Bachelor of Science in Nursing (BSN) program has been ranked the No. 1 accelerated nursing program in Texas by RegisteredNursing.org.
Recent Stories
TTUHSC Experts Receive Junior Investigator Research Grants through Texas Alzheimer’s Research and Care Consortium
Texas Tech University Health Sciences Center (TTUHSC) researchers Aric Logsdon, Ph.D., and Jonathan Singer, Ph.D., received Junior Investigator Research Grants from the Texas Alzheimer’s Research and Care Consortium (TARCC).
CPRIT Awards TTUHSC Researcher $1.4 Million Cancer Grant in Efforts to Expand Rural Clinical Trials
The Cancer Prevention and Research Institute of Texas (CPRIT) awarded a $1.4 million grant to Erin Barr, M.D., a clinician of pediatric hematology/oncology and researcher in the School of Medicine at Texas TTUHSC. Barr’s research, “Enhancing access to pediatric oncology clinical trials in West Texas,” received funding under the Recruitment or Retention of Clinical Trialists Award.
Texas Tech University Health Sciences Center’s Klein Selected to Leadership Role by the Texas Pharmacy Association
The Texas Pharmacy Association announced (May 19) the appointment of Mary Klein, Pharm.D., as assistant vice president of Strategic Initiatives and Practice Innovation.
