World Blood Donor Day
In honor of World Blood Donor Day, June 14, let’s look at how blood donations save lives.
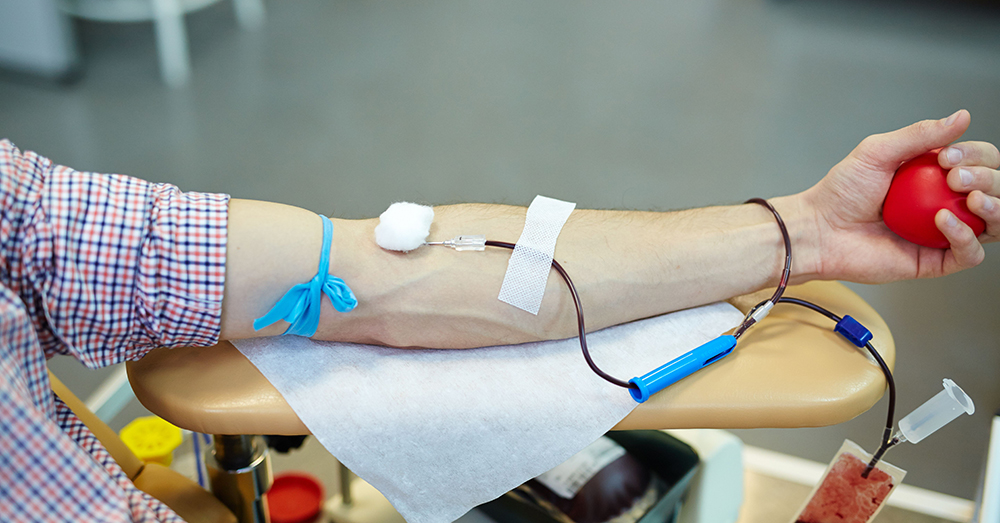
The goal of World Blood Donor Day, June 14 yearly, is to “raise global awareness of the need for safe blood and blood products for transfusion and of the critical contribution voluntary, unpaid blood donors make to national health systems,” according to the World Health Organization.
We spoke with Koy Kubala, M.S. MLS(ASCP)CM MBCM SBBCM, Assistant Professor in the Clinical Laboratory Science Program of the TTUHSC School of Health Professionals, about the importance of blood donation, risks and benefits of donating, and the invaluable services that laboratory scientists provide.
Let’s dive in by discussing how blood is used after being donated.
How Is Donated Blood Used?
Kubala explains that the most common uses for donated blood are for the treatment of anemia, medical trauma commonly seen in emergency rooms, cancer treatments, and for labor and delivery. He also points out that plasma and platelets can be used in people with bleeding disorders.
“We sometimes only think of red cells as being in high demand,” he says, “But in blood banks, platelets are the lowest available product. It’s hard to get people to donate platelets (because of the longer time commitment), but we need them for surgeries and all kinds of procedures.”
Which Blood Types Are in Demand?
There are four major blood groups determined by the presence or absence of two antigens (A and B) on the surface of red blood cells. In addition to the A and B antigens, there is a protein called the Rh factor, which can be either present (+) or absent (–), creating the eight most common blood types (A+, A-, B+, B-, O+, O-, AB+, AB-).
Roughly 45% of people in the United States have type O blood, positive or negative. The proportion is higher among Hispanics (57%) and African Americans (51%). O- red cells can be given to patients of all blood types. Because only 7% of people in the U.S. are type O negative, it’s always in great demand and often in short supply.
“We always want the [blood type] O donors for sure,” Kubala says. “But all are needed.”
Type AB plasma and platelets can be transfused to patients of all blood types. Only 4% of people in the U.S. have AB blood, so these life-saving products are usually in short supply.
Kubala explains that there is more to discover on one’s red cell structure besides just their type.
“If I’m an A+ person, there are other antigens besides your ABO and Rh,” he explains. “We look at full compatibility. If an individual has created an antibody to a specific antigen, we need to find compatibility for that as well. ‘A’ is the tip of the iceberg. We need to look at the full phenotype,” Kubala says.
The Health Risks and Benefits of Donating Blood
Fear is in the eye of the beholder when it comes to blood donations.
“How many times will they stick me and what will I feel like when it’s done?” Kubala says are some of the common perceived risks. The fear of needles is the main issue people face when considering donating blood. There are many safety measures in place, and a donor should feel safe and cared for at the donation facility. Kubala is quick to add that the dreaded needle is a minimal poke that’s far worth the inconvenience.
“Knowing what you’re doing should outweigh any discomfort,” he says. “Fifteen minutes of discomfort isn’t equivalent to someone with sickle cell and has that pain, or a patient who’s anemic, or the pain of a parent who knows their child is on the surgery table.”
There are several health benefits to donating blood, including helping with high blood pressure.
“[Blood donation] stimulates bone marrow to create more fresh red cells, donating can also decrease the risk of cancer,” he explains.
Research has also shown that donating blood helps balance iron levels and helps prevent heart attack and stroke. Donations can serve in a preventative way also, because your blood is tested for any issues before being accepted.
“You get to review your health panel,” he explains, which includes cholesterol, triglycerides
and blood pressure. Clearly, the reasons to donate outweigh the reasons not to.
Blood: The Common Denominator
Currently in the United States, there is no substitute for blood products. Kubala explains that there are other countries with different regulations, who will substitute other products for human blood. These products can cause damage, Kubala warns, and the negative side effects, such as kidney failure, far outweigh the positives.
“Blood crosses economic and racial lines,” Kubala says. “We all bleed the same color.”
Kubala reflects on the powerful effects a random act of kindness such as donating blood can have.
“You may never know who you donated to, but they’re going to be grateful,” he says.
TRUST this Teaching Tool for Clinical Laboratory Science (CLS) Students
Kubala created and uses the acronym TRUST with his CLS students who are working toward a career as health professionals.
- T: Think about the lives you are going to touch and help save by working in the blood bank.
- R: React when a provider or a patient needs your blood bank expertise and lifesaving skills.
- U: Understand that you are going to work hard every day and every sample you work with is a patient and someone’s loved one.
- S: Hold yourself to the highest of standards by being a professional at all times.
- T: Be a team player. It takes more than just one person to save a life and we must all be able to work together.
With such passionate professionals in the lab and in the classroom, it should be an inspiration for all of us to do our part for the common good. Donating blood is an easy way to make a big difference.
Related Stories
38th Student Research Week Successful at Showcasing Secrets of Immune Defense
Student researchers at TTUHSC had the opportunity to showcase their presentation skills at the 38th Annual Student Research Week Feb. 25 – 27.
Celebrating Veterans: TTUHSC’s General Martin Clay’s Legacy of Service and Leadership
From his initial enlistment in the Army National Guard 36 years ago to his leadership in military and civilian health care management roles, Major General Martin Clay’s career has been shaped by adaptability, mission focus and service to others.
Texas Tech University Health Sciences Center School of Nursing Named Best Accelerated Bachelor of Science in Nursing Program in Texas
The TTUHSC School of Nursing Accelerated Bachelor of Science in Nursing (BSN) program has been ranked the No. 1 accelerated nursing program in Texas by RegisteredNursing.org.
Recent Stories
TTUHSC Experts Receive Junior Investigator Research Grants through Texas Alzheimer’s Research and Care Consortium
Texas Tech University Health Sciences Center (TTUHSC) researchers Aric Logsdon, Ph.D., and Jonathan Singer, Ph.D., received Junior Investigator Research Grants from the Texas Alzheimer’s Research and Care Consortium (TARCC).
CPRIT Awards TTUHSC Researcher $1.4 Million Cancer Grant in Efforts to Expand Rural Clinical Trials
The Cancer Prevention and Research Institute of Texas (CPRIT) awarded a $1.4 million grant to Erin Barr, M.D., a clinician of pediatric hematology/oncology and researcher in the School of Medicine at Texas TTUHSC. Barr’s research, “Enhancing access to pediatric oncology clinical trials in West Texas,” received funding under the Recruitment or Retention of Clinical Trialists Award.
Texas Tech University Health Sciences Center’s Klein Selected to Leadership Role by the Texas Pharmacy Association
The Texas Pharmacy Association announced (May 19) the appointment of Mary Klein, Pharm.D., as assistant vice president of Strategic Initiatives and Practice Innovation.
