Novel Treatment Offers Relief to Peripheral Artery Disease Patients
Texas Tech Physicians First in State to Perform Procedure
Because of the pain caused by peripheral artery disease (PAD), Will D. had for years been unable to work in his yard or enjoy a walk with his wife.
“I couldn’t probably walk a third or a quarter of a mile before I had to stop and rest,” he said.
That changed in July when Will D. underwent a new procedure called DETOURTM. His treatment was administered by Mohammad “Mac” Ansari, M.D., director of structural and interventional cardiology research with the Texas Tech Physicians (TTP) Center for Cardiovascular Health.
PAD is a potentially life-threatening condition caused by the buildup of plaque that narrows and restricts blood flow to the body’s peripheral arteries. The condition affects more than 200 million people across the globe, causing pain, impairing mobility and, in advanced cases, leading to amputation.
Though peripheral arteries are located in the legs, stomach, arms and head, Ansari said when physicians speak about PAD they are generally talking about plaque buildup and thickening that can occur within the superficial femoral artery (SFA) and popliteal arteries that circulate blood to the legs. The condition most often affects patients who have diabetes, hypertension, high cholesterol and a history of smoking. PAD makes it difficult for circulation to reach muscles of the lower extremity, which gives the patient several symptoms, including pain.

“Initially this disease was not thought to be that severe,” Ansari explained. “Now the new research shows it’s not only severe and debilitating, it's also deadly. In the long run, the disease turns into what we call CLI, or critical limb ischemia.”
CLI can be a dire condition because it causes ulcers to develop on the legs. In addition to causing pain, the ulcers often become infected and can lead to amputation. Ansari said many patients die within the first two years after the amputation.
PAD is similar to coronary artery disease that occurs in the heart. However, one of the primary differences between PAD and coronary artery disease is the length of the artery blockage. In coronary artery disease, plaque blocks short segments of the arteries. The plaque blockages that occur with PAD are longer segments that generally measure 15 centimeters or more and often contain calcification or complete obstructions known as chronic total occlusions.
While treatments like angioplasty and stenting are effective for coronary artery disease, they are not as successful in addressing the longer blockages produced by PAD. For that reason, doctors have historically used open bypass surgery to treat the long blockages associated with PAD. Though considered to be a more reliable and durable technique for PAD than angioplasty or stenting, Ansari said many patients are hesitant to undergo open bypass surgery because it requires opening the leg and replacing the blocked portion of the artery with an arterial graft.
As an alternative to open bypass surgery, Ansari and TTP have started offering the DETOURTM procedure, a newly developed method for treating PAD. DETOURTM is a minimally invasive percutaneous (i.e., through the skin) femoropopliteal bypass procedure that utilizes small perforations in the skin to bypass long-segment blockages in the superficial femoral artery.
During the procedure, Ansari makes one small perforation near the top of the leg opposite from the leg requiring treatment, and a second in the patient’s calf. He then guides the DETOUR System through the perforations to the area where the artery is blocked and establishes connections between the artery and vein. One connection is made above the blockage and one below the blockage.
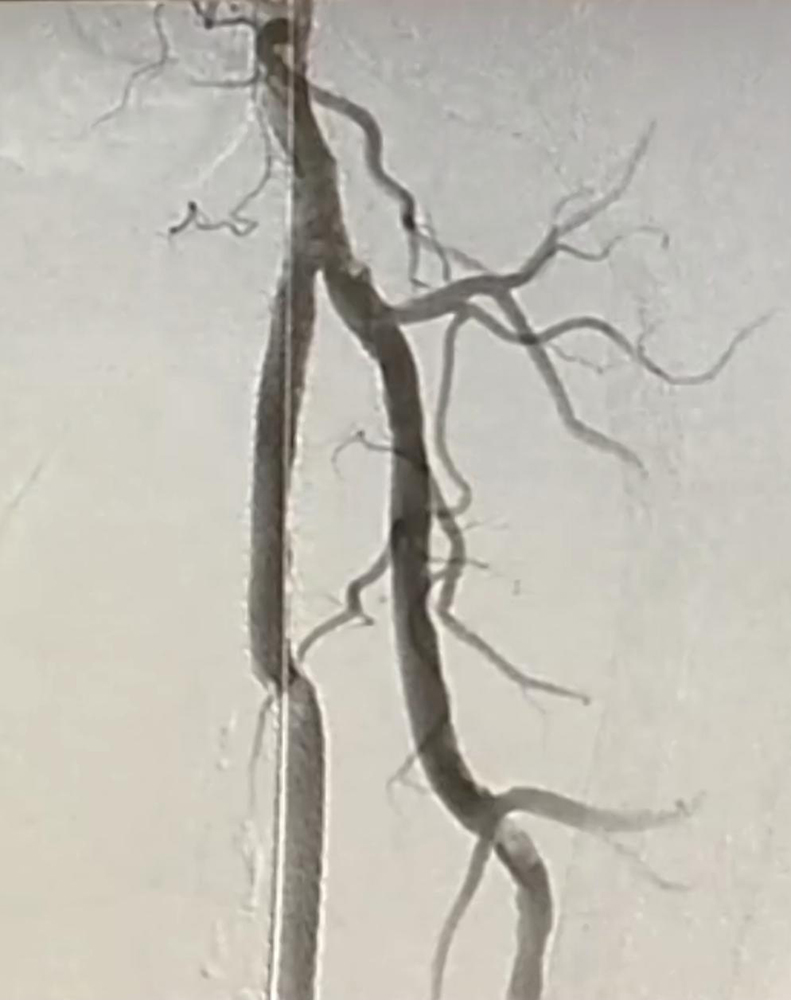
Through these connections, Ansari constructs a long tube by connecting two or three stent grafts. The stent graft tube is started in the artery above the blockage, connects to the vein next to the artery and then returns to the artery below the blockage. This new pathway re-directs oxygen-rich blood around the diseased part of the artery and restores blood flow to the patient’s lower leg and foot.
Recovery time is minimal with the DETOURTM procedure and Will D. said pain was not an issue. Eight days after undergoing treatment he was mowing his lawn.
“Right now I probably just walk and do whatever I want to,” Will D. added. “I’ve been out in the yard working and it’s really not bothering me; there’s no soreness, no hurting in my leg.”
The DETOURTM procedure is being used more frequently in other parts of U.S. and in Europe. Unlike other novel medical procedures that often are available in larger cities like Dallas, Houston or San Antonio, Ansari said he has not heard of anyone else performing the treatment in Texas. He credits university leadership for having the vision and ambition to provide all the latest research, technology, treatment and therapy models to its communities.
“Just imagine somebody suffering from this disease, and then not only do you provide them relief, you provide them their quality of life back. What could be better than that?”
Related Stories
38th Student Research Week Successful at Showcasing Secrets of Immune Defense
Student researchers at TTUHSC had the opportunity to showcase their presentation skills at the 38th Annual Student Research Week Feb. 25 – 27.
Celebrating Veterans: TTUHSC’s General Martin Clay’s Legacy of Service and Leadership
From his initial enlistment in the Army National Guard 36 years ago to his leadership in military and civilian health care management roles, Major General Martin Clay’s career has been shaped by adaptability, mission focus and service to others.
Texas Tech University Health Sciences Center School of Nursing Named Best Accelerated Bachelor of Science in Nursing Program in Texas
The TTUHSC School of Nursing Accelerated Bachelor of Science in Nursing (BSN) program has been ranked the No. 1 accelerated nursing program in Texas by RegisteredNursing.org.
Recent Stories
TTUHSC Experts Receive Junior Investigator Research Grants through Texas Alzheimer’s Research and Care Consortium
Texas Tech University Health Sciences Center (TTUHSC) researchers Aric Logsdon, Ph.D., and Jonathan Singer, Ph.D., received Junior Investigator Research Grants from the Texas Alzheimer’s Research and Care Consortium (TARCC).
CPRIT Awards TTUHSC Researcher $1.4 Million Cancer Grant in Efforts to Expand Rural Clinical Trials
The Cancer Prevention and Research Institute of Texas (CPRIT) awarded a $1.4 million grant to Erin Barr, M.D., a clinician of pediatric hematology/oncology and researcher in the School of Medicine at Texas TTUHSC. Barr’s research, “Enhancing access to pediatric oncology clinical trials in West Texas,” received funding under the Recruitment or Retention of Clinical Trialists Award.
Texas Tech University Health Sciences Center’s Klein Selected to Leadership Role by the Texas Pharmacy Association
The Texas Pharmacy Association announced (May 19) the appointment of Mary Klein, Pharm.D., as assistant vice president of Strategic Initiatives and Practice Innovation.
