Head Trauma in Children

Laszlo Nagy, M.D., is Texas Tech Physicians pediatric neurosurgeon at Covenant Health System and University Medical Center and an associate professor at Texas Tech University Health Sciences Center.
With the advent of a new school year, and the frenzy that parents and children undergo to meet their obligations, opportunities for accidents are prone to increase. Spilling orange juice at the breakfast table, forgetting to close the garage door and the occasional stubbed toe are few of the many nuances that we often face. While these events are uncannily prophesized by Murphy’s Law – ‘Anything that can go wrong will go wrong’ – some accidents may occur with more certainty than chance. Specifically, accidental head trauma in children, a leading cause of death and disability for those under one year of age, is a malady that we can preemptively combat and potentially avoid.
Most visits to the emergency department for children involve some form of head trauma and are usually due to falls, motor vehicle accidents or sports injuries. The younger the child is, the more likely that child will suffer long-term injuries with higher mortality rates than those of older children. Adjunctly, motor-vehicle accidents have higher mortality rates than other forms of head trauma. Without a doubt, the increased likelihood of sustaining deleterious injuries in younger children is related to their softer skulls, as their bones have yet to fully harden and are easily malleable. Similarly, the force of impact during motor-vehicle accidents lends to quicker, more damaging forms of head trauma.
Nearly 90 percent of head injuries are mild and children are usually back home within 24 hours. The best treatment for mild head injuries involves prolonged rest and observation by parents for symptoms such as fluctuations in consciousness or lethargy. It also is advised to wait a few days before allowing those children to gradually return to physical activities or sports.

Preston D’Souza is a TTUHSC third-year medical student.
On the other hand, severe head injuries generally involve skull fractures, collections of blood underneath the scalp and prolonged losses of consciousness. Immediate emphasis is placed on controlling pressures within the brain and skull while multidisciplinary approaches are used to manage physical and intellectual damage. Sadly, children with severe head injuries may have a mortality rate as high as 20 percent.
Recent research has revealed that a history of head trauma, regardless of mild or severe, may lead to a 50 percent more likelihood of using mental health services or admission to a mental health hospital later in life. Long-term consequences of childhood head injuries are still being investigated, but the risk of future intellectual and mental disabilities cannot be taken lightly.
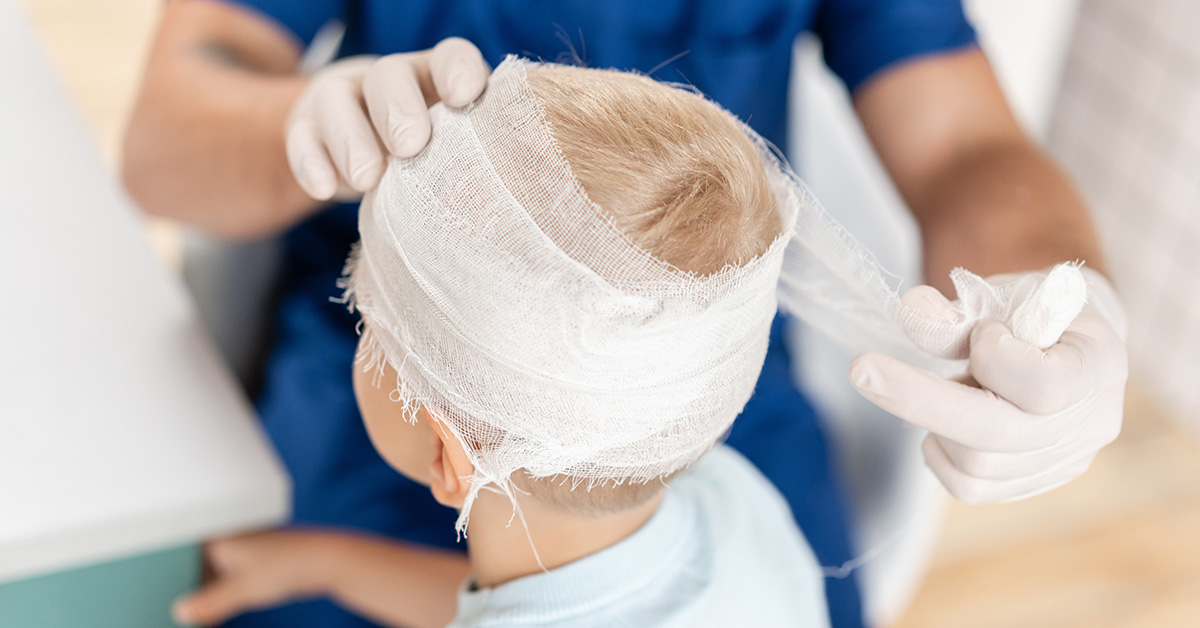
"The best way to avoid a trip to the emergency department is to instill preventive measures that ensure a safe and fun environment for your children."
With these facts in mind, the best way to avoid a trip to the emergency department is to instill preventive measures that ensure a safe and fun environment for your children. While staying mindful of your child’s whereabouts is an obvious mandate, busy moments can lead to lapses in awareness that allow accidents to occur. Utilization of safety guards across stairs and balconies, as well as locking windows and bracing furniture, are few of the common techniques recommended to maintain a child-friendly home. We also advice placing soft material to blunt sharp edges of your furniture.
As always, children under the age of 2 should be in a rear-facing car-seat in the back of the vehicle and should remain in a booster seat between the ages of 8 and 12. Children are only permitted to sit in the front seat at the age of 13 and must have a seat-belt on at all times.
Given this time of year, it is understandable that most children prefer to be outside with their friends, playing sports and riding bicycles. In addition to sunscreen, helmets should always be worn. If your child is of driving age, we recommend a close guardian-child relationship to educate your child on the importance of safe driving protocols as well as education on drinking and driving.
If you are ever in doubt about your child suffering a head injury, please visit your local emergency department as soon as possible.
Have a happy, successful and safe academic year.
Laszlo Nagy, M.D., is Texas Tech Physicians pediatric neurosurgeon at Covenant Health System and University Medical Center and an associate professor at Texas Tech University Health Sciences Center. Preston D’Souza is a TTUHSC third-year medical student.
Related Stories
38th Student Research Week Successful at Showcasing Secrets of Immune Defense
Student researchers at TTUHSC had the opportunity to showcase their presentation skills at the 38th Annual Student Research Week Feb. 25 – 27.
Celebrating Veterans: TTUHSC’s General Martin Clay’s Legacy of Service and Leadership
From his initial enlistment in the Army National Guard 36 years ago to his leadership in military and civilian health care management roles, Major General Martin Clay’s career has been shaped by adaptability, mission focus and service to others.
Texas Tech University Health Sciences Center School of Nursing Named Best Accelerated Bachelor of Science in Nursing Program in Texas
The TTUHSC School of Nursing Accelerated Bachelor of Science in Nursing (BSN) program has been ranked the No. 1 accelerated nursing program in Texas by RegisteredNursing.org.
Recent Stories
TTUHSC Experts Receive Junior Investigator Research Grants through Texas Alzheimer’s Research and Care Consortium
Texas Tech University Health Sciences Center (TTUHSC) researchers Aric Logsdon, Ph.D., and Jonathan Singer, Ph.D., received Junior Investigator Research Grants from the Texas Alzheimer’s Research and Care Consortium (TARCC).
CPRIT Awards TTUHSC Researcher $1.4 Million Cancer Grant in Efforts to Expand Rural Clinical Trials
The Cancer Prevention and Research Institute of Texas (CPRIT) awarded a $1.4 million grant to Erin Barr, M.D., a clinician of pediatric hematology/oncology and researcher in the School of Medicine at Texas TTUHSC. Barr’s research, “Enhancing access to pediatric oncology clinical trials in West Texas,” received funding under the Recruitment or Retention of Clinical Trialists Award.
Texas Tech University Health Sciences Center’s Klein Selected to Leadership Role by the Texas Pharmacy Association
The Texas Pharmacy Association announced (May 19) the appointment of Mary Klein, Pharm.D., as assistant vice president of Strategic Initiatives and Practice Innovation.
