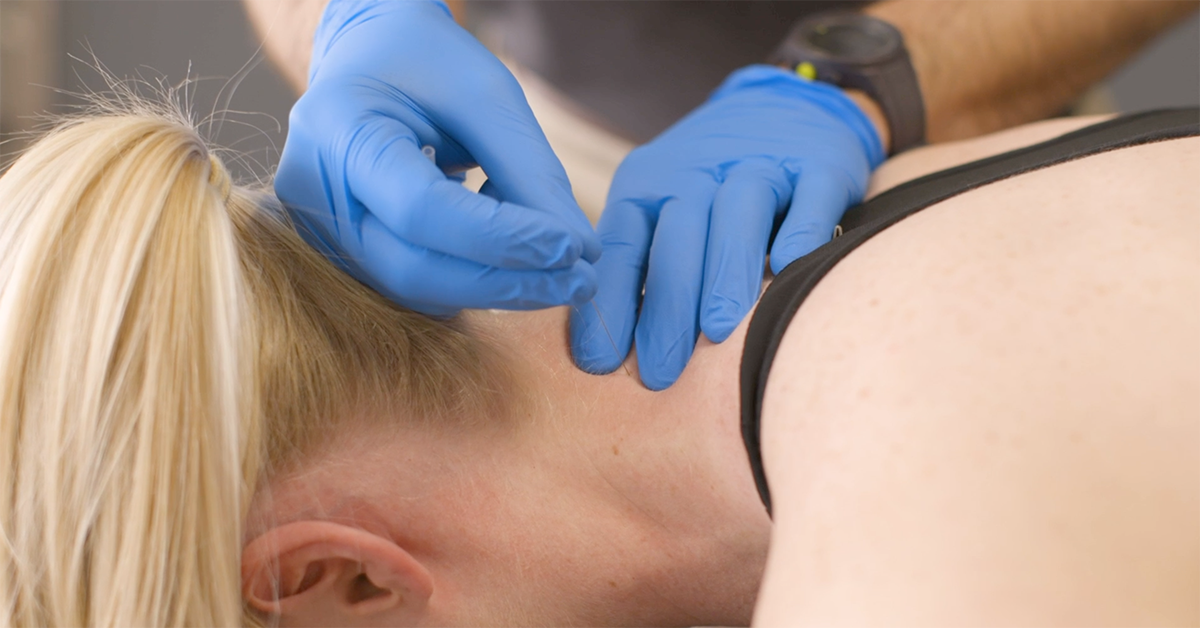
This Needle Can Help Stop Pain — Dry Needling

Gary Kearns, PT, ScD, explains how physical therapists are turning more and more to dry needling to alleviate muscle pain.
Not all needles are alike. Ask Gary Kearns, PT, ScD, assistant professor in the Doctor
of Physical Therapy program in the School of Health Professions, and he gladly explains
how physical therapists are turning more and more to dry needling.
“That's probably the biggest question that I get as a clinician from patients is dry
needling the same as acupuncture? And the answer is no,” Kearns said.
While acupuncture can be used for a number of medical conditions, dry needling is
used by physical therapists to primarily relieve pain and tightness in muscles. By
inserting a needle directly into a trigger point, the needle can release tension in
the surrounding muscles.
“The needles used by acupuncturists and physical therapists are very similar, but
the biggest difference is going to be what your license says you can and can’t do.
From a physical therapy standpoint, we can only treat joints, muscles and the nervous
system,” Kearns said.
The needles used for dry needling are tiny but solid.
“They're different than the type of needles that you would get a flu shot with,” Kearns
said. “A flu shot needle is larger and hollow which allows the flu shot to actually
get into the skin and muscle, whereas the needles we ue are much smaller than that.
That's where the name comes from— it's dry in the sense that you're not injecting
anything. And so, you can get pain relief, without having to having to add any extra
medication to the patient.”
Kearns explained that a physical therapist uses dry needling to relieve pain and relax
the trigger points commonly found to cause musculoskeletal pain and dysfunction. Many
times, a physical therapist will treat chronic conditions like low back pain, headaches
and neck pain, but he said dry needling is simply a tool.
“It’s not going to be the only thing that you receive as a patient to address your
pain and associated impairments,” Kearns said. “It's a component of everything a physical
therapist ay employ to decrease pain, improve flexibility and strength and normalize
function. Dry needling is used to target trigger points and muscles. I like to emphasize
to patients and PT students that dry needling is great for the right person, but requires
a very thorough assessment to address conditions that maybe a contraindication for
choosing dry needling or could increase the chance of a poor response.”
Some of the common considerations to screen include: a fear of needles, infection,
pregnancy (depends on what trimester), blood thinners or a compromised immune system.
“There's a laundry list of things that you have to go through to make sure that everyone
that's coming in is treated appropriately,” Kearns said. “Dry needling works best
when other therapy like joint mobilization, exercise and stretching are combined with
the treatment. It includes the whole gamut of what physical therapy does with dry
needling as a tool used to address the muscle.”
Dry needling has been around since the late ‘60s and early ‘70s. But in terms of being
more commonplace in physical therapy, Kearns said in the U.S., it caught fire in the
last five to 10 years.
“I've been performing dry needling since 2009 when it wasn’t very common, and now,
almost every physical therapy clinic is going to have somebody that does dry needling,”
Kearns said. “The big question is, what's their extra training and how long have they
been using it? Did they just go to a weekend course? Or is it their passion? And obviously,
that's, that's my passion. That's where I do my research which focuses on the safety
of dry needling. I didn't get into physical therapy thinking I would ever be doing
anything invasive. And here we are sticking needles of people. You've always got to
be concerned with ensuring the safety of each patient to maximize outcomes and minimize
potential side effects. You don't ever want to send the patient away worse than when
they came in. Looking for the right expert who has training and asking your health
provider questions is key.”

Dry needling can have potential side effects with potential bruising and soreness
as the most common. But Kearns said the upside of dry needling can far surpass the
possible side effects. If a patient has tight spots in a muscle, the muscle essentially
is staying contracted, and it will not relax. And as a result, it basically keeps
this chemical soup there that produces pain. Physical therapists look to identify
those trigger points. Patient education is key, however.
“We want to make sure that patients know going in eyes wide open, what could go wrong,
but also what steps we take to ensure that it's safe,” Kearns said. “What is appealing
to patients is that it is possible after three to four visits to see results.”
Related Stories
38th Student Research Week Successful at Showcasing Secrets of Immune Defense
Student researchers at TTUHSC had the opportunity to showcase their presentation skills at the 38th Annual Student Research Week Feb. 25 – 27.
Celebrating Veterans: TTUHSC’s General Martin Clay’s Legacy of Service and Leadership
From his initial enlistment in the Army National Guard 36 years ago to his leadership in military and civilian health care management roles, Major General Martin Clay’s career has been shaped by adaptability, mission focus and service to others.
Texas Tech University Health Sciences Center School of Nursing Named Best Accelerated Bachelor of Science in Nursing Program in Texas
The TTUHSC School of Nursing Accelerated Bachelor of Science in Nursing (BSN) program has been ranked the No. 1 accelerated nursing program in Texas by RegisteredNursing.org.
Recent Stories
TTUHSC Experts Receive Junior Investigator Research Grants through Texas Alzheimer’s Research and Care Consortium
Texas Tech University Health Sciences Center (TTUHSC) researchers Aric Logsdon, Ph.D., and Jonathan Singer, Ph.D., received Junior Investigator Research Grants from the Texas Alzheimer’s Research and Care Consortium (TARCC).
CPRIT Awards TTUHSC Researcher $1.4 Million Cancer Grant in Efforts to Expand Rural Clinical Trials
The Cancer Prevention and Research Institute of Texas (CPRIT) awarded a $1.4 million grant to Erin Barr, M.D., a clinician of pediatric hematology/oncology and researcher in the School of Medicine at Texas TTUHSC. Barr’s research, “Enhancing access to pediatric oncology clinical trials in West Texas,” received funding under the Recruitment or Retention of Clinical Trialists Award.
Texas Tech University Health Sciences Center’s Klein Selected to Leadership Role by the Texas Pharmacy Association
The Texas Pharmacy Association announced (May 19) the appointment of Mary Klein, Pharm.D., as assistant vice president of Strategic Initiatives and Practice Innovation.
